 |
 |
AbstractPurposeTo evaluate the incidence and risk factors of post-treatment intracranial hemorrhage of brain metastases from hepatocellular carcinoma (HCC).
Materials and MethodsMedical records of 81 patients who have been diagnosed of brain metastases from HCC and underwent surgery, radiosurgery and/or whole brain radiotherapy (WBRT) between January 2000 and December 2013 were retrospectively reviewed.
ResultsIntracranial hemorrhage was present in 64 patients (79%) at the time of diagnosis. Median value of alpha-fetoprotein (AFP) level was 1,700 ng/mL. The Eastern Cooperative Oncology Group (ECOG) performance status for 20 patients was greater than 2. Fifty-seven patients underwent WBRT and the others were treated with surgery and/or radiosurgery without WBRT. During follow-up, 12 events of intracranial hemorrhage after treatment were identified. Three-month post-treatment hemorrhage rate was 16.1%. Multivariate analyses revealed that ECOG performance status, AFP, and WBRT were associated with post-treatment hemorrhage (p = 0.013, 0.013, and 0.003, respectively). Kaplan-Meier analysis showed that 3-month post-treatment hemorrhage rate of new lesion was higher in patients treated without WBRT, although statistical significance was not reached. (18.6% vs. 4.6%; p = 0.104). Ten of 12 patients with post-treatment hemorrhage died with neurologic cause.
IntroductionBrain metastases from hepatocellular carcinoma (HCC) were very rare [1,2]. However, with the development of neuroimaging studies and improved survival due to the recent advanced therapy to the liver, the incidence has been increasing [3,4]. Brain metastases from HCC are well-known to be accompanied by intracranial hemorrhage at the time of diagnosis. Its incidence has been reported to be 42.8%-74.7% [2,5,6,7].
Whereas optimal management of intracranial hemorrhage from brain metastases has not been established, surgical resection, radiosurgery and whole brain radiotherapy (WBRT) were reported to have own role in the control of the hemorrhagic brain metastases [8,9,10]. Regarding the brain metastases from HCC, Han et al. [11] reported that 30% of the patients with brain metastases from HCC experienced post-treatment hemorrhage after treatment, so recurrent bleeding was the most problematic event during the management of the patients with brain metastases. However, few studies were reported addressing the control of intracranial hemorrhage of the brain metastases from HCC. Recently, Yamakawa et al. [10] reported that WBRT could prevent intracranial hemorrhage. However, this study enrolled only 15 patients and the patients undergoing WBRT were compared with those receiving conservative management only.
In this study, authors evaluated the incidence and risk factor of post-treatment intracranial hemorrhage (defined as hemorrhagic brain metastases developed after initial treatment to brain metastases), and the impact of WBRT in the control of hemorrhage of the brain metastases from HCC.
Materials and MethodsAfter Institutional Review Board approval, medical records of 105 patients who have been diagnosed with brain metastases from HCC between January 2000 and December 2013 were retrospectively reviewed. The patients who received conservative treatment only and who did not complete WBRT were excluded. A total of 81 patients were enrolled in this study. All patients were diagnosed as brain metastases radiologically using computerized tomography or magnetic resonance imaging.
Clinical data including presenting symptoms, performance status, liver function, whether primary lesion controlled or not, presence of extracranial metastases, number of brain lesion, treatment modality and clinical courses were assessed. Because there was no prospective protocol, the patients were under the variable follow-up schedule depending on the physicians. In general, the patients underwent brain images when there was a change in neurologic symptoms. The presence of post-treatment hemorrhage was identified by reviewing all follow-up brain images of the patients. Post-treatment hemorrhage was defined as progression of hemorrhage in the initial lesion, or newly developed hemorrhagic brain metastases. Neurologic death was defined following the study by Patchell et al. [12].
Time to intracranial hemorrhage (TTH) after treatment was calculated from the first day of any active treatment for brain metastases until the radiologic evidence of intracranial hemorrhage. Log-rank test for each prognostic factor was applied to compare the Kaplan-Meier curves for TTH. Cox proportional hazard model analysis was used for multivariate analysis. Log minus log survival plots were used for identifying proportional hazards assumptions. A chi-square test was used to examine the association between categorical variables. A p-value less than 0.05 was considered to indicate a statistically significant difference. Analyses were performed using PASW Statistics ver. 18.0 for Windows (SPSS Inc., Chicago, IL, USA) and the R Project for Statistical Computing ver. 3.1.2.
Results1. Patient characteristicsA total of 81 patients were treated with surgery, radiosurgery or WBRT for brain metastases from HCC. Median age was 56.3 years. Motor weakness (48.1%) was the most frequent symptom followed by headache (32.1%) at the time of diagnosis of brain metastases. Intracranial hemorrhage was detected in 64 patients (79.0%). Brain metastasis presented as a single lesion in 37 patients. Median value of alpha-fetoprotein (AFP) level was 1,700 ng/mL and primary tumor was controlled in 33 patients. Seventy-six patients had extracranial metastases, and the lung was the most frequent involved organ (n = 74). Transcatheter arterial chemoembolization (TACE), surgical resection, percutaneous ethanol injection therapy (PEIT), radiofrequency ablation (RFA), transplantation and/or radiation therapy were performed for the primary therapy to the liver. Chemotherapy was given to 55.6% of the patients. The Eastern Cooperative Oncology Group performance status (ECOG PS) for 20 patients was greater than 2. Child-Pugh classification was evaluated as A for 65 patients, B or C for 16 patients (Table 1).
2. TreatmentFifty-seven patients underwent WBRT. While 47 patients underwent WBRT alone, 7 patients had surgery followed by adjuvant WBRT and 3 patients had radiosurgery plus WBRT. Of 24 patients who had not undergone WBRT, 18 patients had radiosurgery alone, 3 patients had surgery alone, and 3 patients had surgery plus radiosurgery. Details of treatment are summarized in Table 2.
3. Outcome and risk factor analysisMedian length of follow-up was 3.9 months for all patients and 9.3 months for survivors at the last follow-up. During follow-up, 12 post-treatment intracranial hemorrhage were identified. Three-month post-treatment hemorrhage rate was 16.1% (Fig. 1). Median TTH of the patients with post-treatment hemorrhage was 1.9 months (range, 0.2 to 9.0 months). On the univariate analysis, AFP and treatment were significant risk factors (Table 3). Primary tumor control, extracranial metastases and initial hemorrhage were not satisfied with proportional hazard assumption. Using backward selection, ECOG PS, AFP, number of brain lesion, and treatment were incorporated into multivariate analysis. Final analysis with these 4 variables revealed that ECOG PS > 2, AFP ≥ 1,700 ng/mL, and no WBRT were significant risk factors for post-treatment hemorrhage (p = 0.013, p = 0.013, and p = 0.003, respectively). Post-treatment hemorrhage probability according to WBRT was shown in Fig. 2. Distribution of post-treatment hemorrhage lesion according to the treatment was listed in Table 4. Post-treatment hemorrhage of the new lesion was identified in 4 out of 24 patients treated without WBRT, while it was identified in 3 out of 57 patients treated with WBRT. Kaplan-Meier analysis showed that 3-month post-treatment hemorrhage rate of new lesion was higher in patients treated without WBRT (18.6% vs. 4.6%; p = 0.104). When we compared the patients treated with surgery and/or radiosurgery without WBRT (n = 24) and those treated with surgery and/or radiosurgery with WBRT (n = 10), the latter group showed lower 3-month post-treatment hemorrhage rate although there was not statistical significance (30.9% vs. 0%; p = 0.107).
4. Cause of death and recurrent intracranial hemorrhageOverall survival was 3.4 months (95% confidence interval [CI], 0.0 to 6.8) for patients with post-treatment hemorrhage and 4.0 months (95% CI, 3.2 to 4.9) for patients without it (p = 0.236). Of 73 patients who were dead at last follow-up, cause of death was identified as neurologic for 45 patients or systemic for 28 patients. Thirty-five of 61 patients (57.4%) without post-treatment hemorrhage died with neurologic cause, while 10 of 12 patients (83.3%) with post-treatment hemorrhage died with neurologic cause (p = 0.114).
Discussion and ConclusionIn our study, post-treatment hemorrhage of brain metastases from HCC was observed in 15% of patients with 3-month rate 16.1%. ECOG PS > 2, AFP ≥ 1,700 ng/mL, and no WBRT were significant risk factors for post-treatment hemorrhage.
Recently, Yamakawa et al. [10] reported that radiotherapy could prevent intracranial hemorrhage in patient with brain metastases from HCC. In this study, however, the patients undergoing WBRT were compared to those receiving conservative treatment only. In our study, the patient treated with WBRT had lower 3-month post-treatment hemorrhage rate than those treated with surgery and/or radiosurgery without WBRT. Besides, post-treatment hemorrhage was not confined to the initial hemorrhage lesion. Post-treatment hemorrhage rate in the new lesion was higher in patients treated without WBRT, although statistical significance was not reached. Moreover, surgery and radiosurgery could not guarantee to prevent intracranial hemorrhage outside of the target lesion, WBRT would be effective to prevent it in the 'whole brain'.
Generally, more frequent follow-up with brain imaging was done in patients undergoing radiosurgery than WBRT alone. One might argue that frequent follow-up could result in the early detection of the asymptomatic intracranial hemorrhage. To refute this assumption, we compared the post-treatment hemorrhage rate while excluding the patients treated WBRT alone. The patients treated with surgery and/or radiosurgery without WBRT had higher 3-month post-treatment hemorrhage rate than those treated with surgery and/or radiosurgery with WBRT although statistical significance was not reached. In this sense, we can conclude that WBRT prevent bleeding of brain metastases from HCC unbiased by follow-up strategy.
In this study, overall survival was not different in relation to post-treatment hemorrhage. Prognostic factors for overall survival of the patients with brain metastases from HCC were identified as ECOG PS, Child-Pugh class, AFP level, and number of brain lesion in our previous report [7]. Considering the advanced stage of disease, the impact of the recurrent hemorrhage on the overall survival might be limited. However, recurrent hemorrhage could be associated with neurologic death. Although the causal relationship between post-treatment hemorrhage and death was not evident due to the retrospective nature of our study, 10 of 12 patients with post-treatment hemorrhage died with neurologic cause. As uncontrolled recurrent hemorrhage eventually results in neurologic deficit, control of intracranial hemorrhage could be important in the management of brain metastases from HCC.
Major limitation of this study is the insufficient follow-up data of the patients with poor survival outcome and inconsistent follow-up strategy according to the treatment modality due to the retrospective nature of the study. Post-treatment hemorrhage rate of the patients treated with WBRT alone could be underestimated. As discussed earlier, the interpretation of the results should be done with caution. Moreover, single institutional data and heterogeneous population are other limitations of the study. However, considering low incidence of brain metastases from HCC, this is the first report evaluating the post-treatment hemorrhage of brain metastases from HCC with substantial number of population.
In conclusion, post-treatment hemorrhage occurs in 15% of the patients with brain metastases from HCC even after the active treatment, such as surgery, radiosurgery and/or WBRT. Poor ECOG PS, higher AFP, and no WBRT were risk factors for post-treatment hemorrhage. WBRT should be considered to prevent post-treatment hemorrhage in the treatment of brain metastases from HCC.
References1. Tunc B, Filik L, Tezer-Filik I, Sahin B. Brain metastasis of hepatocellular carcinoma: a case report and review of the literature. World J Gastroenterol 2004;10:1688–1689, PMID: 15162554.
2. Chang L, Chen YL, Kao MC. Intracranial metastasis of hepatocellular carcinoma: review of 45 cases. Surg Neurol 2004;62:172–177, PMID: 15261518.
3. Rahbari NN, Mehrabi A, Mollberg NM, et al. Hepatocellular carcinoma: current management and perspectives for the future. Ann Surg 2011;253:453–469, PMID: 21263310.
4. Shao YY, Lu LC, Cheng AL, Hsu CH. Increasing incidence of brain metastasis in patients with advanced hepatocellular carcinoma in the era of antiangiogenic targeted therapy. Oncologist 2011;16:82–86, PMID: 21212425.
5. Hsieh MJ, Lu CH, Tsai NW, et al. Prediction, clinical characteristics and prognosis of intracerebral hemorrhage in hepatocellular carcinoma patients with intracerebral metastasis. J Clin Neurosci 2009;16:394–398, PMID: 19147364.
6. Jiang XB, Ke C, Zhang GH, et al. Brain metastases from hepatocellular carcinoma: clinical features and prognostic factors. BMC Cancer 2012;12:49PMID: 22292912.
7. Kim KS, Kim K, Chie EK, et al. Prognostic stratification of brain metastases from hepatocellular carcinoma. J Neurooncol 2014;120:209–214, PMID: 25052350.
8. Yoo H, Jung E, Gwak HS, Shin SH, Lee SH. Surgical outcomes of hemorrhagic metastatic brain tumors. Cancer Res Treat 2011;43:102–107, PMID: 21811426.
9. Redmond AJ, Diluna ML, Hebert R, et al. Gamma Knife surgery for the treatment of melanoma metastases: the effect of intratumoral hemorrhage on survival. J Neurosurg 2008;109:99–105, PMID: 19123895.
10. Yamakawa Y, Moriguchi M, Aramaki T, et al. Brain metastasis from hepatocellular carcinoma: The impact of radiotherapy on control of intracranial hemorrhage. Hepatol Res 2014;12 03 [Epub]. http://dx.doi.org/10.1111/hepr.12457.
11. Han JH, Kim DG, Park JC, Chung HT, Paek SH, Chung YS. Little response of cerebral metastasis from hepatocellular carcinoma to any treatments. J Korean Neurosurg Soc 2010;47:325–331, PMID: 20539790.
12. Patchell RA, Tibbs PA, Walsh JW, et al. A randomized trial of surgery in the treatment of single metastases to the brain. N Engl J Med 1990;322:494–500, PMID: 2405271.
Fig. 2Post-treatment hemorrhage probability according to whole brain radiotherapy (WBRT). TTH, time to hemorrhage.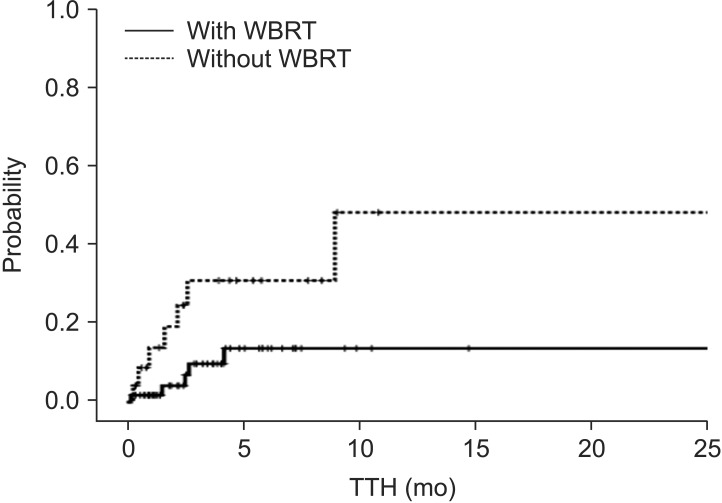
Table 1Clinical characteristics of 81 patients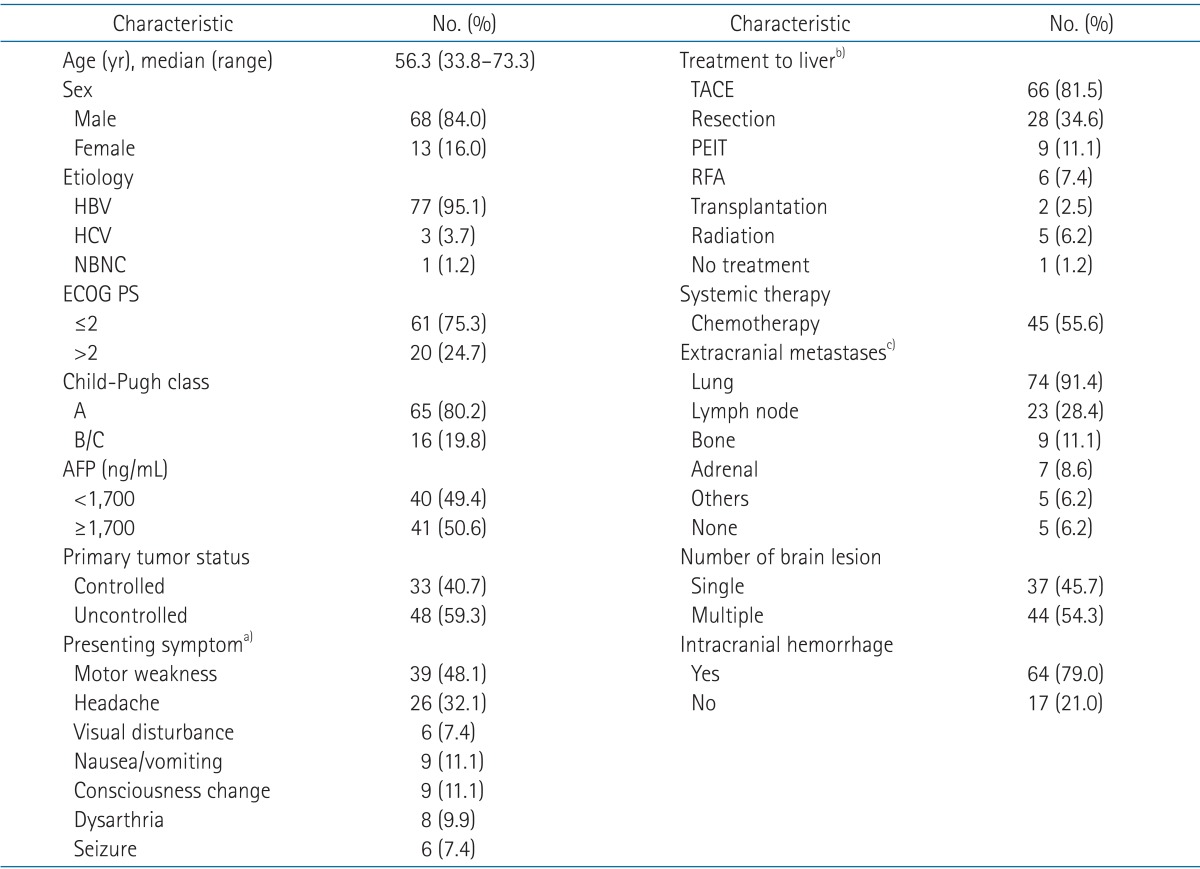 HBV, hepatitis B virus; HCV, hepatitis C virus; NBNC, non-B and non-C; ECOG PS, Eastern Cooperative Oncology Group performance status; TACE, transcatheter arterial chemoembolization; PEIT, percutaneous ethanol injection therapy; RFA, radiofrequency ablation. a)Each symptom was counted regardless of other symptoms of each patient. b)Patients could be treated with more than one modalities. c)Each metastasis was counted regardless of metastasis of other site. |
|
||||||||||||||||||||||||||||||||||||||||

 |
 |